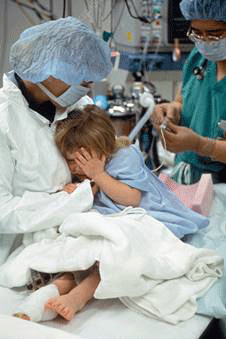
Procedural Anxiety
Consider the following:
- Build a rapport with the child through playful interaction.
- Address any parental anxiety and outline ways in which caregivers can help the child, or offer to let the parent leave the room if they prefer. Using a treatment room for procedures is recommended to avoid the child developing negative associations with the exam rooms used for routine patient care.
- If Child Life specialists are available, their expertise may reduce or eliminate the need for medical analgesia and anesthesia.
- Consider non-pharmacological relaxation approaches to help children before and during procedures. These may include aromatherapy, music, massage, and local application of vibration or ice to dull sensation to the skin that will be poked. Infants may benefit from sucking on a bottle or oral sucrose. Breastfeeding and placing the baby skin-to-skin (“kangaroo care”) can help but may be more challenging for positioning.
- When possible, engage parents in holding the child in positions of comfort and distracting the child with cartoons, relaxation apps, songs, bubbles, etc.
- Plan ahead for the appropriate level of analgesia and anesthesia. Consider options such as ice, vibration, and/or topical anesthetics to dull sensation to the area. Consider pre-administration of over-the-counter analgesics like ibuprofen or acetaminophen.
- In the outpatient setting, benzodiazepines are not used except for extreme anxiety. The primary care clinician can consider a small dose of oral or intranasal midazolam (Versed) or lorazepam (Ativan) 30-60 minutes prior to a procedure. Due to the risk of respiratory depression and paradoxical reactions, use benzodiazepines only in a clinical setting where monitoring and interventions are available.
- Make a plan for what happens when the procedure ends. Simple rewards such as fun Band-Aids, stickers, colorful casts, or a popsicle can help kids feel better after the procedure. Praise children for being courageous.
Families should know what degree of pain to expect after the procedure and how they can help the child. Encourage the family to familiarize themselves with resources (see below) that help with anxiety or pain.
Resources
Information & Support
For Professionals
Managing Procedural Anxiety in Children (NEJM)
Ten-minute video that presents a thoughtful, step-wise approach to reducing anxiety during clinic visits and medical procedures;
New England Journal of Medicine.
Vulnerable Patients (APA)
A brief article discussing distraction, exposure therapy, and other approaches to reducing pediatric anxiety in the medical
setting; American Psychological Association.
Helping Children and Families Cope with Needle Sticks (Children's National) ( 504 KB)
504 KB)
Behavioral strategies that help to mitigate anxiety about needles and needle‐related pain.
For Parents and Patients
Getting a Shot: You Can Do It! (Sid the Science Kid/PBS)
A 28-minute YouTube video for kids about why and how we get vaccinations.
Medical Procedures and Pain: Helping Your Child (University of Michigan)
Concise guide to help families understand and reduce their child's anxiety and pain in during shots and procedures.
A Fun Way to Ease Kids’ Anxiety About Medical Procedures (University of Michigan)
An introduction to medical play.
Preparing Your Child (Duke Children's Hospital & Health Center) ( 288 KB)
288 KB)
A stepwise approach, organized by age of the child, for parents to prepare children for hospitalizations and procedures.
Using Comfort Positions During Stressful Events (St. Jude Children's Research Hospital)
Show family members how to hold children in comfort positions during medical procedures.
Relaxation Workbook (Primary Children's Hospital) ( 407 KB)
407 KB)
Self-administered relaxation exercises and pages for reflection.
Pain Management Workbook (Primary Children's Hospital) ( 408 KB)
408 KB)
Self-administered pain management exercises and pages for reflection.
Practice Guidelines
Fein JA, Zempsky WT, Cravero JP.
Relief of pain and anxiety in pediatric patients in emergency medical systems.
Pediatrics.
2012;130(5):e1391-405.
PubMed abstract
An AAP guideline to pediatric analgesia and anxiolysis in the EMS and emergency department settings, including information
relevant to children with developmental disabilities. Reaffirmed Nov 2015.
Patient Education
Let's Talk About: Helping Your Child Cope with Medical Procedures (Intermountain Healthcare) ( 1.9 MB)
1.9 MB)
A printable handout about preparing and supporting the child during painful procedures. Illustrates comfort positions for
parents holding their child and gives examples of encouraging words.
Let's Talk About... Pain Management Techniques for Special Needs Children (Spanish and English)
A 2-page printable handout with tips for identifying potential sources of pain in a child who is unable to tell you what is
wrong and how to manage pain without medications; Intermountain Healthcare.
Let's Talk About... Counterstimulation Techniques Using Sensory Distraction (Spanish & English)
A 2-page printable handout with simple examples of counterstimulation techniques using sight, sound, smell, taste, and touch;
Intermountain Healthcare.
Helpful Articles
Dastgheyb S, Fishlock K, Daskalakis C, Kessel J, Rosen P.
Evaluating comfort measures for commonly performed painful procedures in pediatric patients.
J Pain Res.
2018;11:1383-1390.
PubMed abstract / Full Text
Authors & Reviewers
| Author: | Jennifer Goldman, MD, MRP, FAAP |
| Reviewers: | Sheldon Furst, MD |
| Holly Moss-Rosen |
| 2019: update: Jennifer Goldman, MD, MRP, FAAPA |
| 2018: update: Mary Steinmann, MD, FAAP, FAPAA |
| 2016: first version: Douglas Nelson, MDR |
Page Bibliography
Dastgheyb S, Fishlock K, Daskalakis C, Kessel J, Rosen P.
Evaluating comfort measures for commonly performed painful procedures in pediatric patients.
J Pain Res.
2018;11:1383-1390.
PubMed abstract / Full Text
Fein JA, Zempsky WT, Cravero JP.
Relief of pain and anxiety in pediatric patients in emergency medical systems.
Pediatrics.
2012;130(5):e1391-405.
PubMed abstract
An AAP guideline to pediatric analgesia and anxiolysis in the EMS and emergency department settings, including information
relevant to children with developmental disabilities. Reaffirmed Nov 2015.


 Get Help in Rhode Island
Get Help in Rhode Island